Did you know that dangerous bacteria from your mouth can get into your bloodstream, travel through your body, and increase your chances for many health problems throughout your system?
 As a part of my participation in the American Dental Association’s Institute for Diversity in Leadership, I am working on a project that includes introducing an oral-health curriculum to primary-care and other medical clinicians, with a goal of making medical providers aware of the benefits of early dental intervention and prevention. In my research work for this project, I have come across many cases of oral bacteria’s causing problems in other parts of the body, and I would like to share one case with you.
As a part of my participation in the American Dental Association’s Institute for Diversity in Leadership, I am working on a project that includes introducing an oral-health curriculum to primary-care and other medical clinicians, with a goal of making medical providers aware of the benefits of early dental intervention and prevention. In my research work for this project, I have come across many cases of oral bacteria’s causing problems in other parts of the body, and I would like to share one case with you.
A study published in the Journal of American College of Obstetricians and Gynecologists in 2010 reported a case of stillbirth caused by Fusobacterium nucleatum originating in the mother’s mouth. The woman, who had gum disease, developed an upper–respiratory-tract infection, which was followed by a stillbirth a few days later. F. nucleatum was isolated from the placenta and the fetus, and further examination revealed that the mother had the same bacterial clone in the dental plaque under her gum. Analysis concluded that the F. nucleatum may have moved from the mother’s mouth to the uterus when her immune system was weakened by the respiratory infection.
California Dental Association Foundation’s “Evidence Based Guidelines for Oral Health During Pregnancy and Early Childhood” suggests that pregnancy is not a reason to defer routine dental care or treatment of oral health problems, because, during pregnancy, continuing routine oral care presents less fetal or maternal risk than going without such care. Good oral health and control of oral disease protect the mother’s health and quality of life and can reduce the transmission of pathogenic bacteria from mother to fetus.
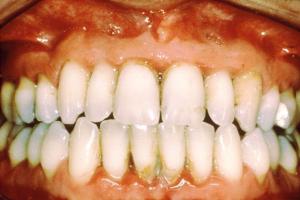
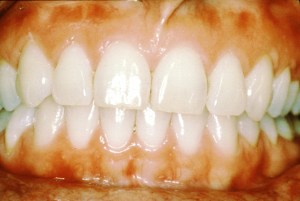
The inflammation that occurs with periodontal disease plays an increasingly significant role in oral–systemic disease connections. Aspiration of oral bacteria, for example, can be associated with pneumonia, and gum disease is strongly linked with diabetes. There is also evidence of periodontal health’s being linked to obesity, coronary-artery disease, metabolic syndrome, menopausal problems, and adverse pregnancy outcomes.
It is vital that the entire team of the patient’s health-care providers—dentist, hygienist, internist, cardiologist, endocrinologist, and obstetrician—be educated regarding the patient’s risk factors, in order for them to work with one another to provide the patient with optimal care.
The entire subject of oral-systemic-linked disease is too broad to discuss in this blog, but I encourage readers to educate themselves about this subject, to stay informed regarding their overall health, and to take an active role in discussion and communication with the provider physicians who are treating them.